How to treat warts and condyloma acuminata? Do not apply ointments indiscriminately! Identify the types clearly, 3 categories of methods for rapid eradication
Doctor, I have small bumps on the back of my hand. I've been applying ointment for half a month without improvement. Could it be genital warts? I have cauliflower-like bumps in my private area. Online sources say soaking them in vinegar can help. Is that reliable? Every day in the clinic, I encounter patients who treat warts incorrectly. Although common warts and genital warts are both caused by HPV infection, they differ in location, harm, and treatment methods. Using the wrong medication is not only ineffective but may also worsen the condition. Today, as a gynecologist, I will thoroughly explain the treatment plans for both conditions to help you avoid misunderstandings and achieve proper, complete removal.
First, highlight the key points: Common warts mostly grow on the hands, feet, and face, and are considered "minor skin issues"; genital warts appear in private areas, are highly contagious, prone to recurrence, and require professional treatment. First, identify the type, then discuss treatment to avoid taking the wrong path.
First, Distinguish: Do You Have "Common Warts" or "Genital Warts"? A 30-Second Self-Check
Comparison Item | Common warts (commonly known as "verruca vulgaris") | Condyloma acuminatum |
HPV genotype | Low-risk types 1, 2, 4, etc. (non-carcinogenic) | Low-risk types 6 and 11 (non-carcinogenic, but highly contagious) |
Location of growth | Back of the hand, fingers, soles of the feet (plantar warts), face (flat warts) | Vulva, vaginal orifice, perianal area, vaginal/cervical lining |
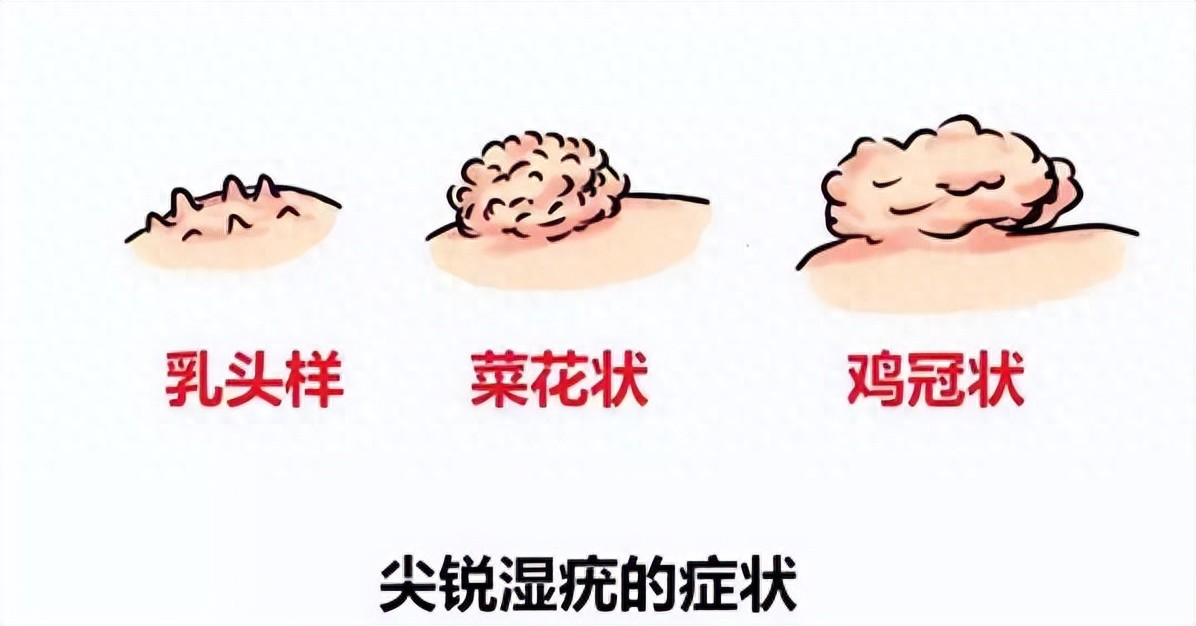
Morphology | Rough and raised, resembling small fleshy granules, with a color similar to the skin. | Cauliflower-like, cockscomb-like, papillary, pale red or skin-colored |
Infectious | Weak (contact transmission, such as sharing towels) | Strong (primarily transmitted through sexual contact, but can also be indirectly transmitted) |
For example, 26-year-old Xiao Lin developed three rough small bumps on the back of his hand, which are common warts; while 32-year-old Sister Zhang developed cauliflower-like bumps on her vulva, diagnosed as genital warts—both appear to be "warts," but the treatment plans are vastly different.
II. How to Treat Common Warts? 3 Types of Methods, Simple and Effective (Suitable for Hands, Feet, and Face)
Common warts are usually painless and non-itchy, but if they appear in visible areas affecting appearance or on the soles of the feet (plantar warts) causing pain while walking, these three treatment options can be considered, with most cases cleared in 1-2 sessions
1. Physical Therapy: Rapid Wart Removal, Suitable for Most People
CryotherapyThe wart is frozen with liquid nitrogen at minus 196°C, causing it to necrotize and fall off, suitable for small warts on the back of the hand and fingers (diameter < 1cm).
Advantages: Fast (done in 10 minutes), inexpensive (tens of yuan per session); Disadvantages: May cause pain, blistering, and scabbing that falls off in 2-3 weeks.
Laser TherapyUsing high-temperature laser to burn off warts is suitable for plantar warts on the soles of the feet (deeper) and flat warts on the face.
Advantages: Precise, less likely to leave scars; Disadvantages: Painful (requires local anesthesia), costs several hundred yuan per session, large warts may require 2 sessions.
2. Topical medications: suitable for individuals who are afraid of pain and have small warts.
Imiquimod CreamApply 2-3 times per week; it works by activating local immunity to clear warts, suitable for flat warts and small hand warts.
Note: Slow onset of action (requires 4-8 weeks), do not apply to broken skin, may cause mild redness and swelling.
Salicylic Acid OintmentApply once daily to soften the wart and promote its shedding, suitable for plantar warts on the soles of the feet.
Caution: Avoid applying to surrounding healthy skin to prevent corrosion.
3. Other Methods: Special circumstances may be selected.
Wart Clamp RemovalThe doctor directly removes small warts with hemostatic forceps (requiring local anesthesia), suitable for single small warts on fingers.
Photodynamic TherapyApplying medication followed by light therapy is suitable for large areas of flat warts on the face. The advantage is minimal scarring, while the disadvantage is the high cost (several thousand yuan per session).
CaseXiao Wang, a 28-year-old, developed plantar warts on the soles of his feet, which caused pain while walking. After one session of laser treatment, the warts were completely removed. He fully recovered within two weeks without any scarring.
III. How to Treat Genital Warts? 4 Steps of Standardized Treatment to Avoid Recurrence (Key Points!)
Genital warts located in the private area are highly contagious and prone to recurrence. Self-treatment is not advisable; a two-step approach of "removing warts + preventing recurrence" must be followed. The treatment cycle typically lasts 1-3 months.
1. Remove warts first: 3 types of physical/chemical methods
Laser / Cryotherapy / ElectrocauterySimilar to common warts, laser ablation, cryotherapy with liquid nitrogen, or electrocautery can be used to remove the warts, which is suitable for visible warts in the vulvar and perianal areas.
Note: Warts in the vagina and cervix require special instruments for manipulation to avoid mucosal damage.
Topical medicationsThe doctor prescribes specialized medications, such as:
Podophyllotoxin Tincture: Apply twice weekly to erode warts (contraindicated in pregnant women).
Interferon gel: Apply after wart removal to reduce recurrence.
Photodynamic TherapySuitable for recurrent cases with multiple warts. Apply medication first, then undergo phototherapy to clear latent viruses. The recurrence rate is 50% lower than that of laser treatment.
2. Key: To prevent recurrence, three things must be done.
Regular follow-upDuring the first to third month after treatment, follow-up examinations should be conducted every two weeks; from the third to sixth month, monthly follow-up examinations are recommended, with prompt management in case of recurrence.
Both partners should be treated simultaneously.Genital warts are transmitted through sexual contact, and partners must be examined; even if no bumps are present, they may still carry the virus. Simultaneous treatment is necessary to avoid cross-infection.
Enhance immunityStaying up late and high stress levels can easily lead to recurrence. Sleeping 7 hours a day, consuming 1 egg + 1 cup of milk daily, and brisk walking 3 times a week can strengthen immunity, making it harder for the virus to "make a comeback."
CaseAfter being diagnosed with genital warts at age 30, Sister Li underwent laser wart removal and applied interferon gel. Her partner also underwent simultaneous examination and treatment. With consistent follow-up for 6 months without recurrence, she has now fully recovered.
IV. Avoid These 3 Treatment Misconceptions to Prevent Worsening the Condition
Myth 1: "Soaking in vinegar or applying folk remedy ointments can remove warts"
Wrong Soaking in vinegar can corrode the skin and folk remedy ointments may contain hormones which not only fail to remove warts but can also cause genital warts to spread and common warts to proliferate
2. Misconception 2: "Once the wart falls off, it's cured; no follow-up is needed."
Wrong! Genital warts have a high latent virus load. The disappearance of warts does not mean the virus is cleared. Without follow-up examination, the recurrence rate exceeds 60%. If common warts are not completely removed, they may also regrow.
3. Misconception 3: "It's easier to just pick off the wart myself."
Wrong! Picking at warts can cause the virus to spread (for example, after picking a wart on the back of the hand, new warts may appear elsewhere on the fingers) and may also lead to bacterial infection and scarring.
Finally, the doctor reminds:
Common warts: If they are not painful or itchy, they can be observed. If they affect daily life, seek treatment at the dermatology department. Most cases can be resolved in one session.
Genital warts Regardless of the size of the warts it is essential to visit the gynecology or dermatology and venereology department of a regular hospital and avoid private clinics
Core Both are HPV infections After treatment boosting immunity less staying up late eating more protein can reduce recurrence and also lower the risk of other HPV infections

If you are currently troubled by "warts," first use the methods mentioned earlier to self-check which type it is, then seek standardized treatment from the corresponding department—don't panic. As long as you choose the right method, whether it's common warts or genital warts, they can be completely cured without resorting to misguided self-treatment!