Is flat wart related to cervical cancer? Both are caused by HPV infection, but one is carcinogenic while the other is not. Do not confuse them.
Doctor, I have flat warts on my face. Does that mean I'm infected with HPV? Could I get cervical cancer? Last week at the outpatient clinic, 28-year-old Xiao Song anxiously asked while holding a mirror—this is a common confusion many people have: flat warts are caused by HPV, and cervical cancer is also related to HPV. Are the two related? Does having flat warts mean you are closer to cervical cancer? Today, as a gynecologist, I will thoroughly explain the relationship between the two, neither exaggerating the risks nor overlooking the details. After reading this, you won't need to worry unnecessarily.
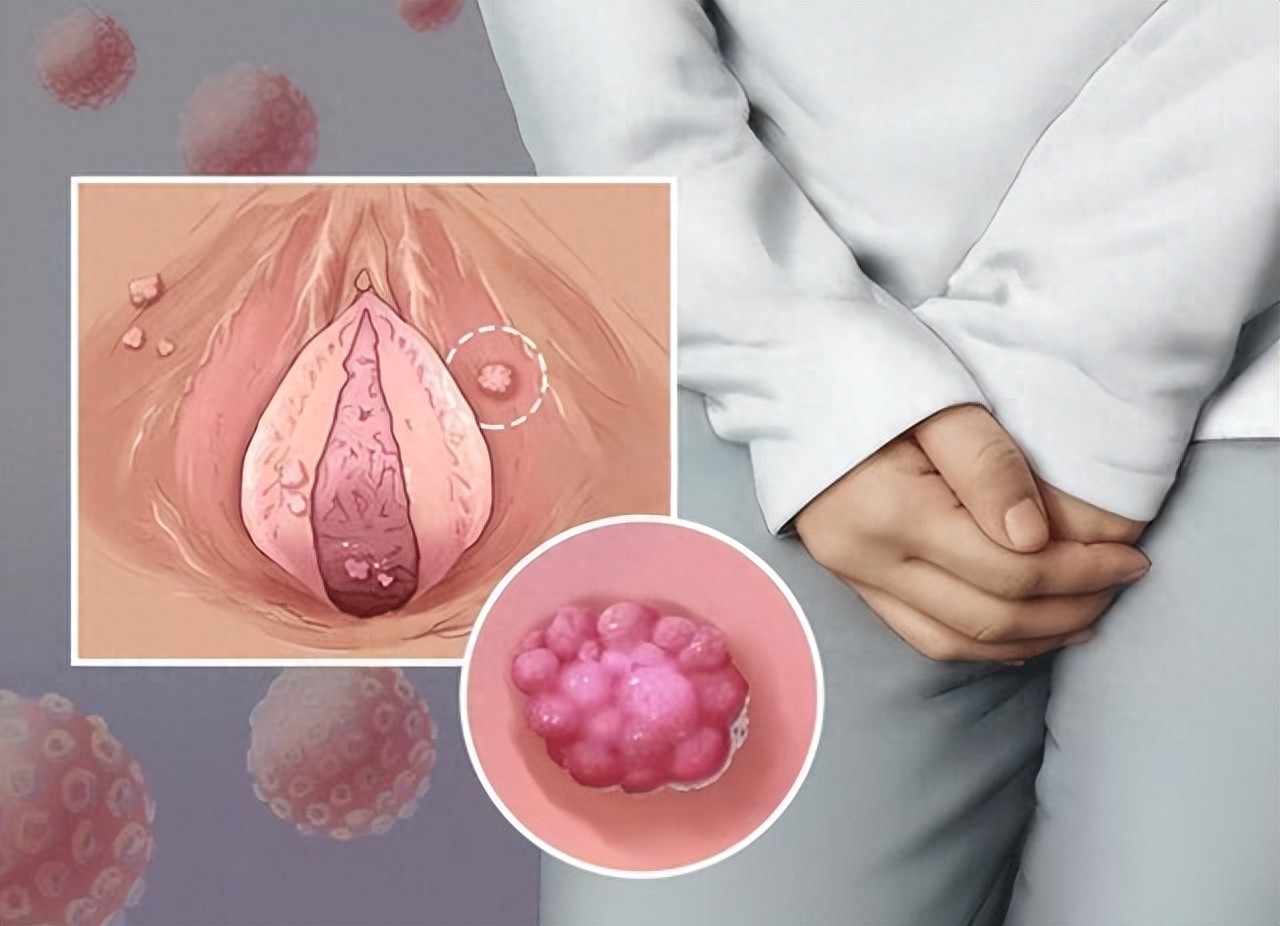
First, the core conclusion:Flat warts and cervical cancer are indeed both caused by HPV (human papillomavirus) infection, but they are caused by completely different "HPV strains"—one is a "low-risk harmless type," and the other is a "high-risk carcinogenic type." There is no direct correlation between them; having flat warts does not directly lead to cervical cancer.。
First, understand: the HPV that causes flat warts and cervical cancer belongs to "different families."
The HPV family comprises over 100 types, which are categorized into two groups based on "carcinogenic risk." The causative agents of flat warts and cervical cancer belong to different categories.
1. The "culprit" of flat warts: low-risk HPV (types 3, 10, 6, 11, etc.)
This type of HPV is completely non-carcinogenic and only infects the skin epidermis, causing benign small bumps on the skin, like "minor troubles on the skin surface." It does not invade reproductive organs such as the cervix or vagina, nor does it cause cancer.
For example, the flat warts on Xiao Song's face are caused by HPV type 3 infection, which only "causes trouble" on the surface of the skin and has no relation to cervical health. Clinically, the risk of cervical cancer in patients with flat warts is no different from that of the general population.
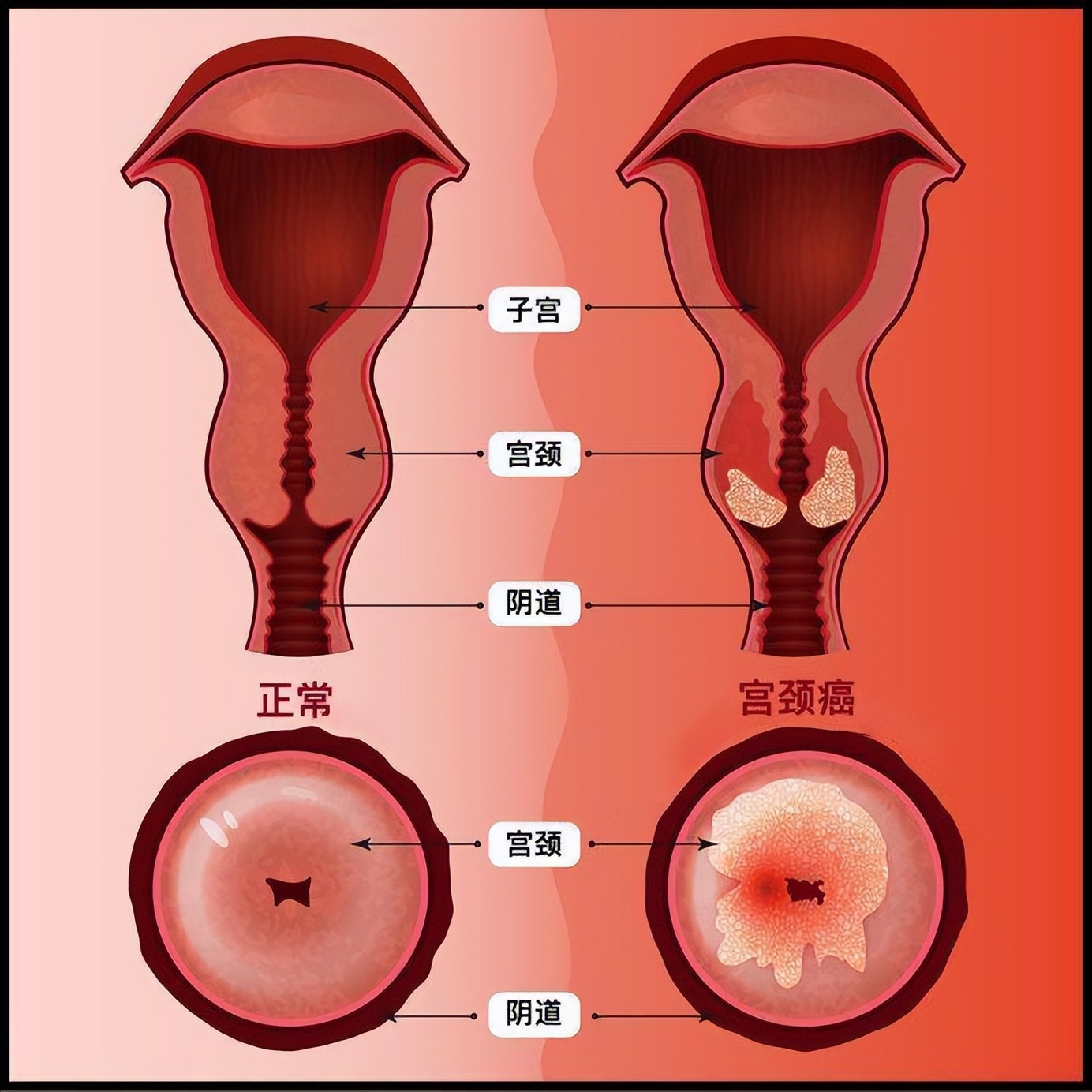
2. The "culprit" of cervical cancer: high-risk HPV (types 16, 18, 52, 33, etc.)
This type of HPV is a "master of carcinogenesis," primarily infecting mucosal tissues such as the cervix and vagina. If the infection persists for more than two years, it gradually damages cervical cells, leading to precancerous lesions and even cervical cancer. Specifically, types 16 and 18 are responsible for over 70% of cervical cancer cases, which is entirely different from the low-risk HPV types that cause flat warts.
Simply put, contracting flat warts is like encountering the harmless troublemakers within the HPV family, while infection with high-risk HPV is akin to facing dangerous criminals. There is no direct connection between the two.
II. Three Key Differences Between the Two, Easy to Understand at a Glance
Comparison Dimensions | Flat Warts | HPV infection associated with cervical cancer |
Site of infection | Superficial skin layer (face, back of hands, arms, etc.) | Cervix, vaginal mucosa |
Symptom Manifestations | Flat, smooth, light brown small bumps, painless and non-itchy, contagious but not malignant | Most cases are asymptomatic, while a few may experience postcoital bleeding or abnormal vaginal discharge. Persistent infection may lead to malignant transformation. |
Degree of harm | Affects appearance, no health risk | May cause cervical cancer and endanger life |
Take a real case: Ms. Wang, 45 years old, had flat warts (HPV type 10) for 10 years. She underwent regular cervical cancer screenings every year, with consistently normal HPV and TCT results. In contrast, her friend, who did not have flat warts, tested positive for HPV16 but did not take it seriously. Three years later, she was diagnosed with high-grade cervical lesions. This clearly demonstrates that these are two entirely separate health issues.
III. Common Misconceptions: Stop Dwelling on These 2 Ideas
Myth 1: "Having flat warts means I am prone to HPV infection and will definitely develop cervical cancer."
Wrong! Infection with low-risk HPV does not mean it is easy to contract high-risk HPV. The transmission routes and infection sites of the two are completely different: flat warts are mainly transmitted through skin contact (such as sharing towels or scratching), while high-risk HPV is primarily transmitted through sexual contact. Infection with low-risk HPV does not increase the risk of contracting high-risk HPV.
2. Misconception 2: "I don't have flat warts, so I won't be infected with high-risk HPV and don't need cervical cancer screening."
Wrong! Most high-risk HPV infections are asymptomatic and unrelated to the presence of flat warts. Women aged 21 and above who are sexually active, regardless of whether they have flat warts, should undergo regular cervical cancer screening (TCT for ages 21-29, HPV+TCT after age 30). This is the only method to detect high-risk HPV infections.
IV. Practical Advice: What to Do If You Have Flat Warts? How to Prevent Cervical Cancer?
1. Regarding flat warts: No need to panic, symptomatic treatment is sufficient.
If it affects appearance: You can go to the dermatology department for cryotherapy or laser treatment, or apply tretinoin cream externally, which can quickly remove it with a low recurrence rate.
Daily Protection: Avoid scratching (to prevent self-infection), do not share towels or washbasins, wash hands frequently, and prevent cross-infection.
Key Reminder: There is no need to test for cervical HPV due to flat warts, as they are unrelated. Do not waste your money.
1. Regarding Cervical Cancer: Focus on Preventing High-Risk HPV, Do These 2 Things Well
HPV vaccination Regardless of whether flat warts are present as long as the age criteria are met bivalent 9-45 years quadrivalent 20-45 years nonavalent 16-26 years priority should be given to vaccination which can directly prevent high-risk HPV infection
Regular screening: Follow age-appropriate standardized screening to detect high-risk HPV infections early. Clearing the infection through immunity or medical intervention can help prevent cervical cancer.
V. Special Circumstances: Be Extra Vigilant If These 2 Situations Occur
When flat warts appear along with symptoms such as bleeding after intercourse or blood in vaginal discharge, do not focus solely on the flat warts. It is important to undergo cervical cancer screening promptly to rule out high-risk HPV infection.
Flat warts recur repeatedly, and the individual has poor immunity (such as diabetics, those who stay up late for long periods): Weak immunity may allow various HPV types to take advantage. It is recommended to undergo cervical cancer screening while treating flat warts, and to improve immunity (eat more protein, reduce staying up late, engage in moderate exercise).
Finally, I want to say: flat warts and cervical cancer are health issues that share a common origin but follow different paths. There is no need to panic if you have flat warts, nor should you ignore cervical cancer prevention just because you don’t have them. If you have flat warts, seek treatment in dermatology. For cervical cancer prevention, rely on "vaccination + screening." The two are clearly divided in their roles and do not interfere with each other.
If you are currently troubled by flat warts or have questions about cervical cancer screening, do not hesitate—address them specifically. The key to health is distinguishing between "minor issues" and "major risks." By responding scientifically, you can achieve both peace of mind and ease of care.