Can high blood sugar levels definitively be diagnosed as diabetes?
Recently, I treated a friend's mother who had been diagnosed with high blood sugar levels two years ago at an external hospital through check-ups and tests, but was not directly diagnosed with diabetes. As a result, the patient has never believed she has diabetes, merely high blood sugar levels!
There haven't been any changes in diet or lifestyle, nor have I taken any hypoglycemic medications. I haven't been monitoring my blood sugar levels regularly, and two years have passed like this.
Recently, I've been feeling unsteady when walking, as if my feet are staggering and I can't keep my balance firmly. However, there are no symptoms of limb weakness or reduced flexibility. Since my husband had limb weakness due to a stroke, I was worried about whether I might also have a stroke, so I came to the hospital for a check-up and was diagnosed with pontine infarction. Although the company isn't very large, it still caused lower limb ataxia and deep sensory perception disorders.
At the same time, it was found that the patient's blood sugar levels were abnormal, with a fasting blood glucose level of 7.3 millimoles per liter. Based solely on this indicator, it wouldn't meet the diagnostic criteria for diabetes.
The patient repeatedly told the doctor that he doesn't have a history of diabetes, but that a doctor had once told him his blood sugar was high, though not high enough to be diagnosed as diabetes!
Fasting blood glucose less than 7.8 millimoles per liter indeed cannot be diagnosed as diabetes.
However, for this group of people, there is already a condition of impaired fasting glucose. The diagnosis of diabetes is not just based on fasting blood glucose levels but also requires testing postprandial blood glucose at 2 hours, and it may even be necessary to perform an oral glucose tolerance test (OGTT).
Latent diabetes generally refers to cases where fasting or postprandial blood glucose at 2 hours (or a positive OGTT test) has already been diagnosed as diabetes, but there are no clinical symptoms of diabetes. It is difficult to detect clinically and often leads to delayed diagnosis and treatment.
The progression from normal blood glucose levels to hyperglycemia and ultimately developing into a confirmed diagnosis of diabetes is a gradual process without a clear boundary line.
Therefore, once individuals with abnormal blood sugar levels are identified, even if they have not reached the diagnostic threshold for diabetes, we should take high importance. It is not only necessary to measure fasting blood sugar but also to measure postprandial blood sugar at 2 hours, and even conduct OGTT and HbA1c screening to early detect diabetic patients in a latent state.
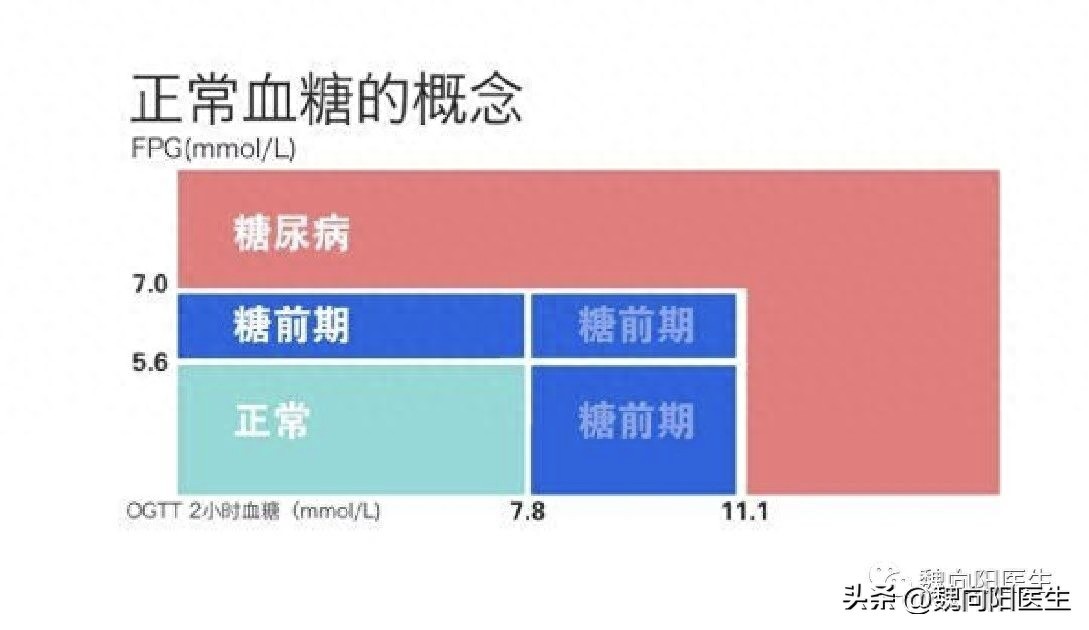
After glucose tolerance screening, individuals who still cannot be diagnosed with diabetes but have exceeded normal blood sugar levels, such as fasting blood sugar > 5.6 mmol/L and ≤ 7.0 mmol/L, and OGTT 2-hour blood sugar > 7.8 mmol/L and < 11.1 mmol/L, can be diagnosed as having prediabetes.
This early diagnosis can help patients understand how far they are from being diagnosed with diabetes and that the rising blood sugar has already begun to cause ultrasound damage to body tissues and organs. At this stage, although medication to lower blood sugar is not necessary, changes should be made in diet and actual actions. Through standardized diabetes education and promotion, patients should be made aware of how to control their blood sugar, thereby avoiding progression to a confirmed diabetes diagnosis.